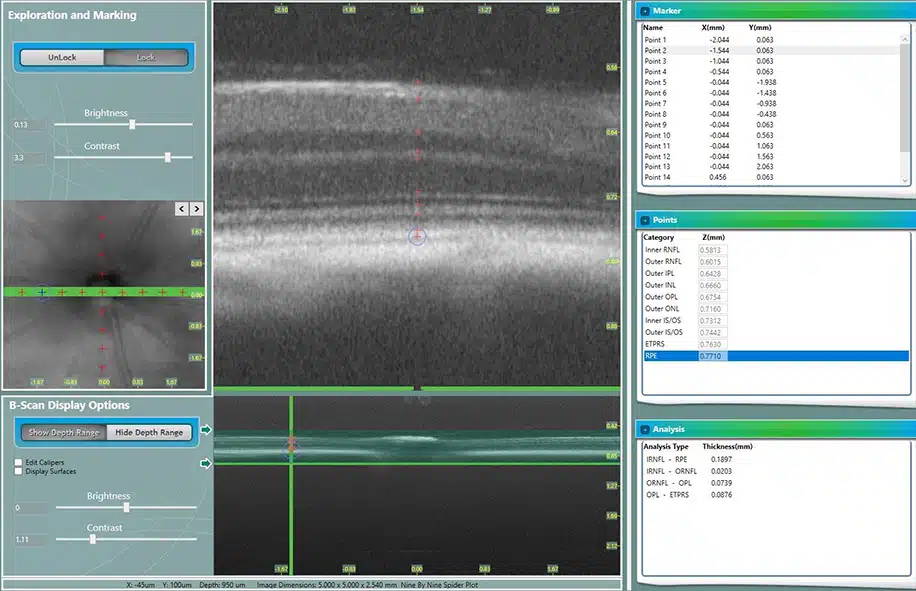
We provide the ability to track disease progression after induction of disease by utilizing optical coherence tomography (OCT), measuring full retinal thickness, the retinal ganglion cell (RGC) layer and nerve fiber layer (RNFL) in real time.
In conjunction with OCT we use electroretinography (ERG) to test retinal functionality. Upon the conclusion of the study, we use histopathology to assess the condition of the retinal ganglion cells and potential protection from your product to RGC and RNFL.
Primary Endpoints in the Optic Nerve Crush Model
Optical Coherence Tomography (OCT)
High quality retinal scanning using the Lecia® SD-OCT allows for accurate retinal thickness measurements of distinct retinal layers.
Electroretinography (ERG)
Our lab uses a proprietary ERG system in collaboration with Cornell University to produce the most accurate ERGs.
Microinfusion Injection Delivery
Confirmation fundus images of each injection procedure that ensures proper delivery of treatment.
Retinal Ganglion Cell Count
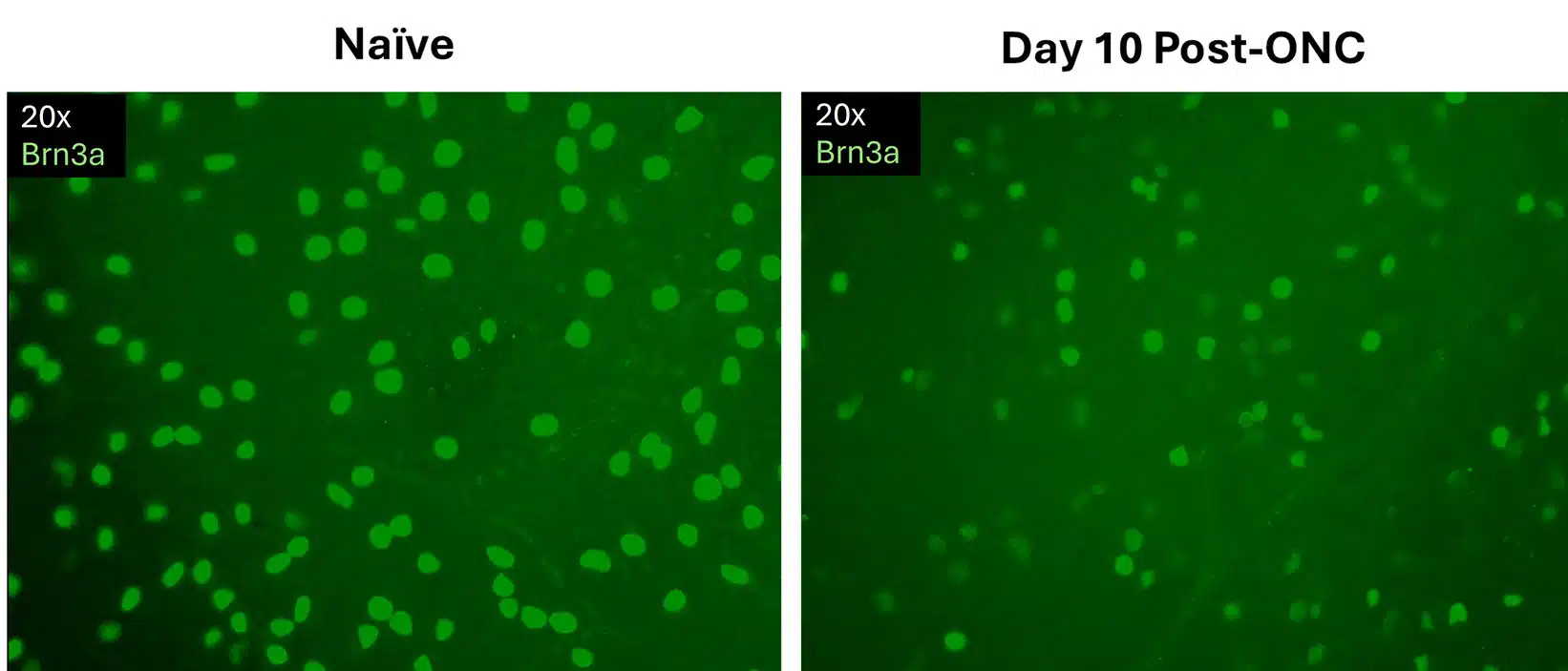
A reduction in total retinal ganglion cell count is a hallmark endpoint in the rodent optic nerve crush model. Cellular loss can be observed qualitatively with representative images as shown or quantitatively used automated image analysis.
Retinal Nerve Fiber Layer Thickness
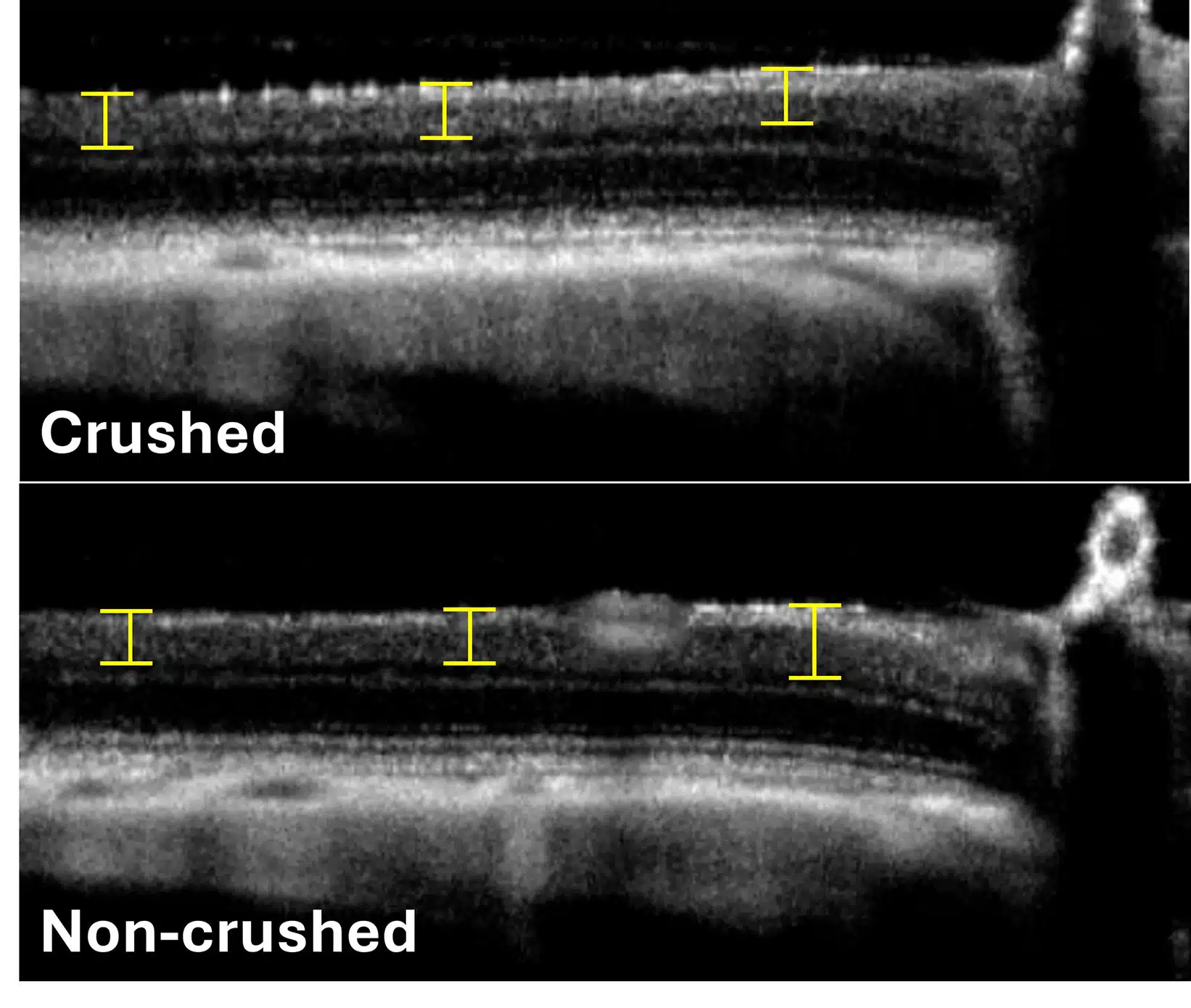
Thinning of the RNFL and inner plexiform layer (IPL) can be measured by OCT in the optic nerve crush model. This read-out enables monitoring over time with repeat measurements while providing robust qualitative and quantitative structural data.
About this model
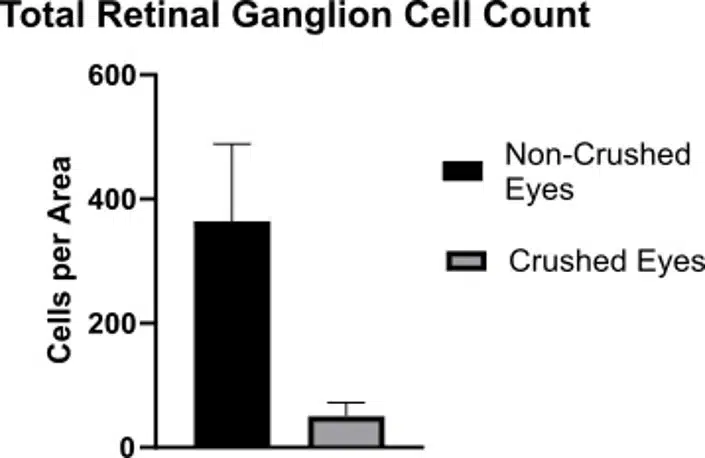
Retinal Ganglion Cell Quantification
Quantification of total retinal ganglion cells per area matches what is observed qualitatively in the fluorescence microscopy images shown above. Additional cellular staining options are available.
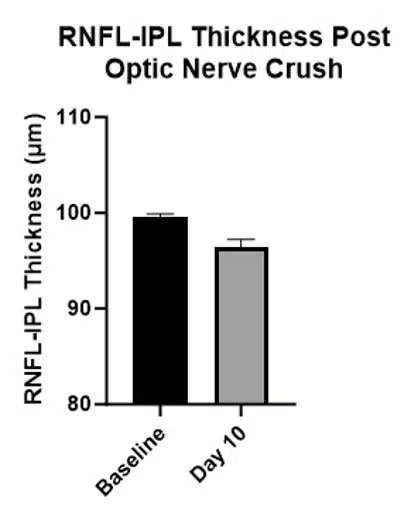
RNFL-IPL Thinning in the Optic Nerve Crush Model
Thinning of the RNFL-IPL in the optic nerve crush model can be observed using OCT and quantified. This enables repeat measurements to obtain a time course of disease onset and progression.
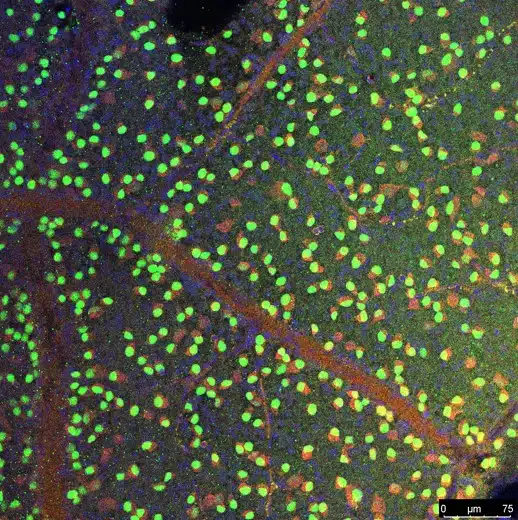
Customized Imaging and Assessments
Retinal flat mounts and histological sections can be processed with a wide variety of stains and antibodies for molecular markets of interest. Inquire about customized assessment needs for your project.